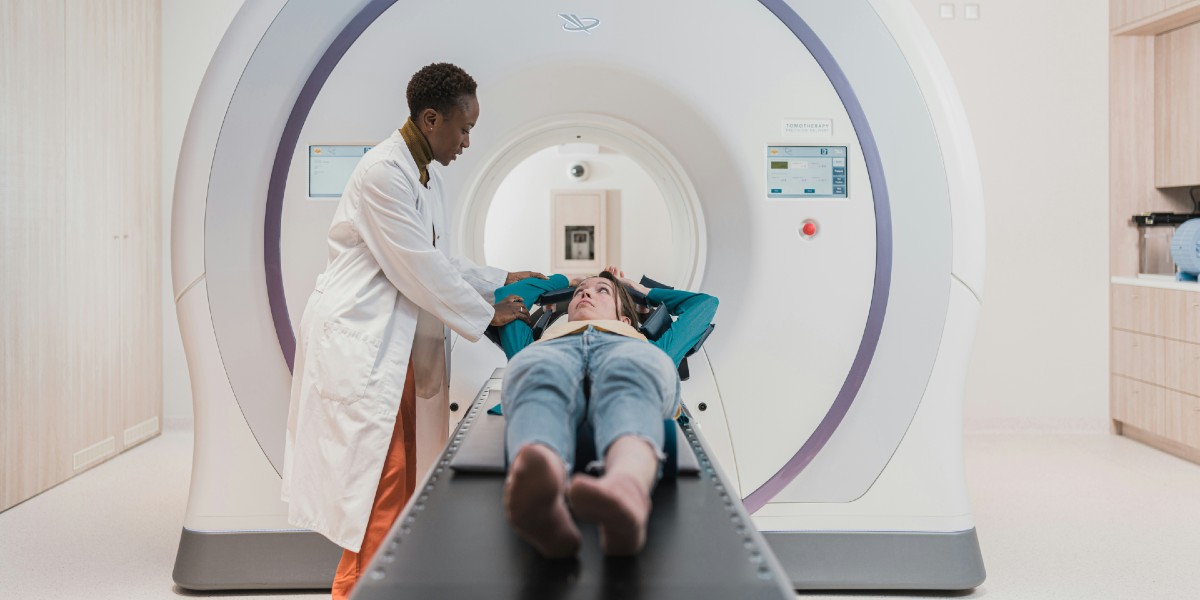
Below, Alexandra Sifferlin shares five key insights from her new book, The Elusive Body: Patients, Doctors, and the Diagnosis Crisis.
Alexandra is a health and science editor for The New York Times Opinion desk. She is a former deputy editor of the health publication Elemental and a staff writer at Time, where she covered medicine and public health.
What’s the big idea?
Each year, millions of Americans leave a doctor’s office with the wrong diagnosis—or no diagnosis at all. It’s a problem that is far more common, and more preventable, than most people realize.
Listen to the audio version of this Book Bite—read by Alexandra herself—in the Next Big Idea App, or buy the book.

1. Nearly every American will suffer from a diagnostic error.
In the United States, diagnostic errors—which can include a delayed diagnosis, a wrong diagnosis, or a missed diagnosis—affect at least five percent of adults every year. According to an influential 2015 report from the National Academies of Sciences, Engineering, and Medicine, most people will experience at least one diagnostic error in their lifetime. Researchers at Johns Hopkins University estimated that close to 800,000 Americans become permanently disabled or die each year because dangerous diseases are misdiagnosed.
That being said, doctors do usually get diagnoses right, with some estimates suggesting around 90 percent of the time. But given there are around 155 million emergency room visits each year and around 1 billion physician office visits, even a low error rate can translate into a lot of affected people. It is worth trying to improve these numbers.
2. Delayed diagnosis is costly for everyone.
The longer a diagnosis takes, the more patients cycle through appointments, tests, and ineffective treatments. The U.S. spends twice as much on health care as comparable countries and yet has worse outcomes. Americans may be less likely to seek medical attention because of cost or because it takes so long to finally get a doctor’s appointment. Sometimes they seek medical attention only when things are quite bad. This is a costly cycle.
“A doctor may have no idea if their diagnosis was right for the patient they saw.”
There is currently no federal reimbursement incentive for hospitals with lower diagnostic error rates. Major health care systems in the U.S. don’t systematically track diagnostic errors. A doctor may have no idea if their diagnosis was right for the patient they saw. If doctors and hospitals were incentivized to reduce diagnostic error rates, and if health care systems tracked the errors that do occur, this would decrease overall costs for everyone involved and more efficiently ensure that patients receive appropriate care.
3. We need doctors back at the bedside.
For centuries, the physical exam was critical for diagnosis and helping doctors gain experience. But as technology advances, many physicians have begun prioritizing new tools over listening to patients and observing their symptoms. A better balance restores the physical exam and patient interaction as the foundation of care, with technology used to confirm or refine what clinicians learn at the bedside. Research suggests that this approach reduces diagnostic errors and creates a more rewarding experience for both doctors and patients.
However, that’s not to say technology isn’t important. It is. Everything from the stethoscope to an ultrasound is important for diagnosis. Now, there is a lot of excitement around artificial intelligence and the ability of large language models to take great amounts of medical information and aid in diagnosis. There are still many unanswered questions and potential overhype of AI, but it might radically change healthcare diagnosis.
4. Diagnostic mistakes arise more from how doctors think than from what they know.
Errors frequently emerge during the reasoning process itself: when uncertainty is handled poorly, alternative explanations are overlooked, or reflection is cut short. Diagnosis is not simply a technical task but a judgment skill.
“Errors frequently emerge during the reasoning process itself.”
Advocates of this view emphasize that such judgment can be strengthened through deliberate training, particularly by prioritizing clinical reasoning in medical education and by creating systems that allow physicians to review outcomes across many cases.
5. A more humane approach to medicine can go a long way.
The National Institutes of Health’s Undiagnosed Diseases Network brings together clinicians and researchers of different disciplines to diagnose some of the most complicated medical mysteries. These experts work together to understand each patient in a holistic way with longer appointments and access to the best technology. They have been able to diagnose many people with rare or even novel diseases.
In speaking with participants for my book, what stood out most was not the specialized tests or advanced tools, but how people were treated. Patients emphasized the humanity of the care—being listened to, taken seriously, and respected. Even those whose diagnostic journeys remain unfinished described the experience as profoundly better than anything they had encountered before.
One woman I profiled spent decades undiagnosed and in severe pain before clinicians at the Undiagnosed Diseases Network spent time with her and her family and discovered that she and her four siblings shared a very rare disease experts hadn’t known about before.
Enjoy our full library of Book Bites—read by the authors!—in the Next Big Idea App: